
Frozen shoulder, also known as adhesive capsulitis, is a painful condition that affects the shoulder joint. It is characterized by a gradual and progressive loss of range of movement and stiffness in the ball-and-socket (glenohumeral) joint of the shoulder, which can make it very difficult to perform everyday tasks, such as washing your hair and fastening a bra behind the back. An initial trigger such as a minor injury or illness can result in a cascade of inflammation within the shoulder which then leads to adhesions forming and subsequent gross restriction of range of movement.
The condition typically follows a three-stage pattern:

Frozen shoulder can affect people of all ages, but it is most common in people aged 40 to 60. It is also more common in women than in men. People with Type-1 (insulin dependent) diabetes, a history of previous shoulder injuries, or individuals who have had to keep their shoulder immobilised for a period of time, i.e. after surgery or following an arm fracture, are at increased risk of developing frozen shoulder.
The main symptoms of frozen shoulder are:


The pain may be felt in the shoulder itself or may radiate down the arm to the elbow or hand. The stiffness may make it difficult to perform everyday tasks, such as dressing, bathing, and reaching overhead.

There is no specific test for frozen shoulder. The clinical diagnosis is usually made based on the patient's medical history and physical examination. The specific examination findings include restriction when placing hands behind the head, limitation of range of movement when reaching behind the back and limitation when attempting to raise the hands above the head. The doctor may order imaging tests, such as X-rays, ultrasound or MRI scans, to rule out other causes of shoulder pain. On ultrasound assessment your doctor will be looking for excess fluid within the biceps tendon sheath and the ball-and-socket joint.
Contact Us 020 8004 6659Treatments aim to relieve inflammation, pain and improve function. Treatment options may include:
Corticosteroid injections can be a highly effective way of reducing inflammation and pain associated with a frozen shoulder. The two main injection options include
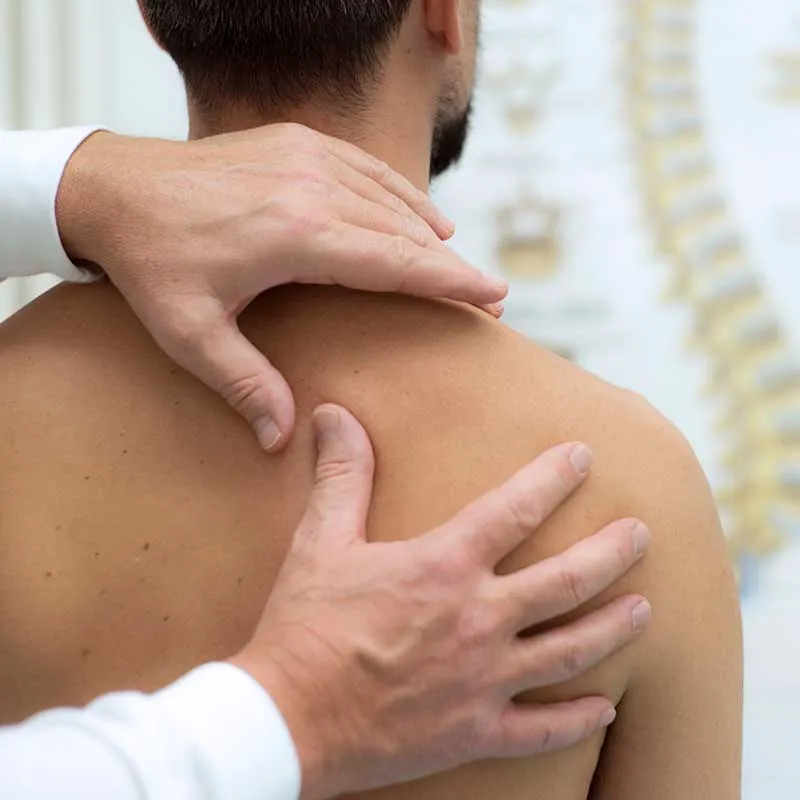
At The Joint Injection Clinic, these injections are performed after a thorough consent process, whereby the risk and benefits of the procedure are discussed in detail with your doctor. The experienced medical doctor will then place you in a side-lying position with the affected shoulder upmost and with the hand of the affected shoulder placed on the opposite side of the chest. The shoulder is cleaned using a cleaning solution to ensure that the procedure is performed under sterile conditions. Local anaesthetic is injected from the skin to the joint under ultrasound guidance. After giving the local anaesthetic a few minutes to take effect, the standard shoulder joint injection or hydrodilatation procedure is performed with a small dose of steroid and local anaesthetic (and sometimes water/saline), targeting the back part of the ball and socket joint.
The injection itself is normally completed within 30-60 seconds (3-5 minutes for the hydrodilatation procedure), after which a plaster is applied and post-injection advice is given. The patient is advised to look out for any signs of infection, specifically to check whether the local area becomes red, hot, tender, swollen or if they develop a fever. If this occurs then the patient is asked to contact the clinic immediately at which time a formal reassessment will occur and if needed oral antibiotics can be prescribed. The patient is also warned that following any injection they may notice a short-term worsening or flare in their symptoms after the local anaesthetic has worn off (4-5 hours). This may last for 3-5 days and the patient is advised to consider icing of the area using an ice pack for 10-15 minutes every hour as required.
Most cases of frozen shoulder resolve on their own within 1 to 3 years. However, treatment can help to relieve pain and improve function during this time.If you are experiencing pain and stiffness in your shoulder, it is important to see a doctor to get a diagnosis and discuss treatment options.