
Ankle osteoarthritis (OA) is a relatively common condition that affects the cartilage, a smooth, flexible tissue that cushions the ends of bones in the knee joint. Over time, the cartilage in the ankle joint can wear down and become rough, leading to pain, stiffness, inflammation and loss of function in the knee.
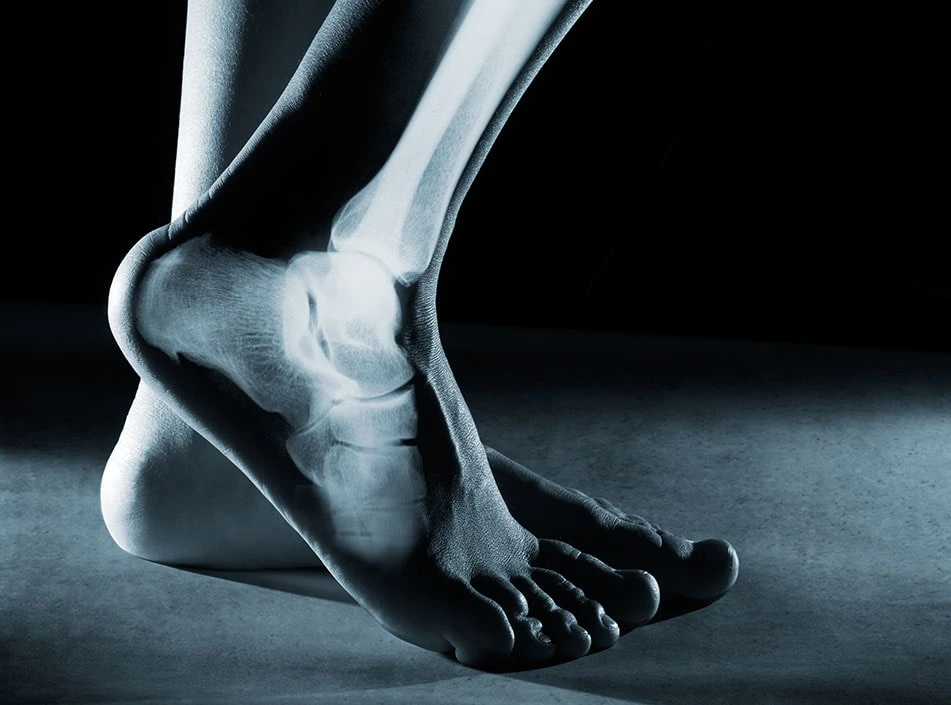
Ankle osteoarthritis is most common in adults over the age of 50, and the risk of developing it increases with age. Women are more likely than men to develop ankle osteoarthritis, especially after menopause. Other factors that increase the risk of ankle osteoarthritis include:
Excess weight puts extra stress on the ankle joint.
Injuries to the ankle, such as combined bone and cartilage (osteochondral) injuries, ligament rupture, fractures or dislocations, can increase the risk of developing osteoarthritis later in life.
Having a family history of osteoarthritis increases your risk of developing it yourself.
The main symptoms of ankle osteoarthritis include:

Symptoms may worsen gradually over time and may fluctuate depending on the level of activity. Activities that involve weight-bearing, such as walking, climbing stairs, or standing for long periods, can aggravate the pain and discomfort.
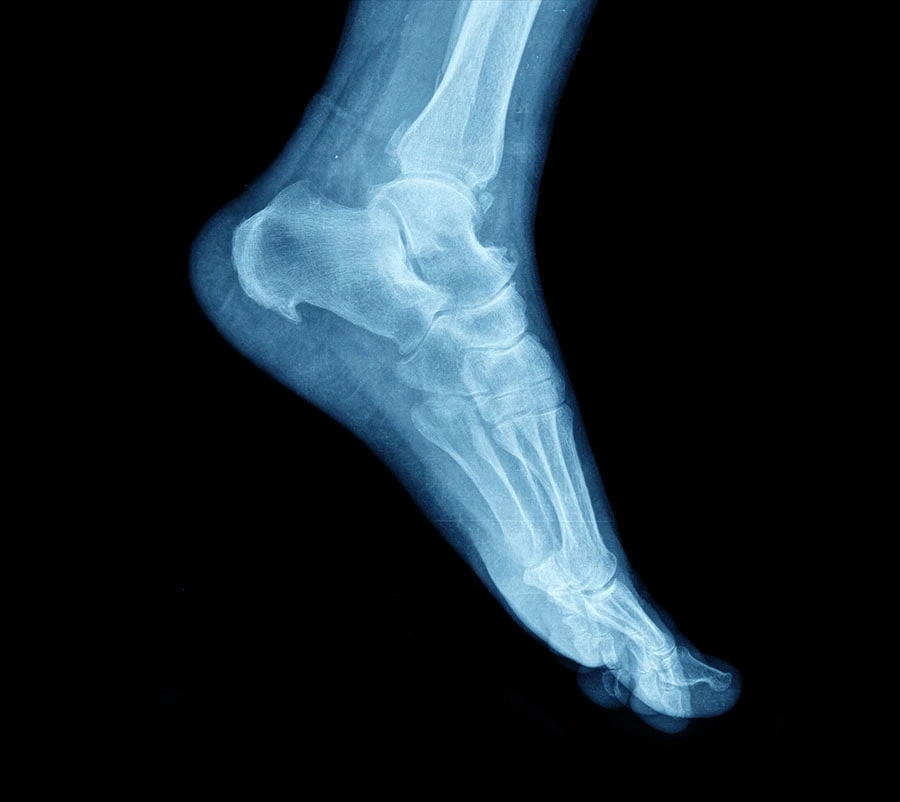
Diagnosis of ankle osteoarthritis typically involves a physical examination, medical history review, and imaging tests.
Treatment for ankle osteoarthritis focuses on managing symptoms, slowing the progression of the condition, and improving function. Non-surgical treatments are usually tried first, and surgery is considered if non-surgical measures fail to provide adequate relief.


The injection itself is normally completed within 30-60 seconds, after which a plaster is applied and post-injection advice is given. The patient is advised to look out for any signs of infection, specifically to check whether the local area becomes red, hot, tender, swollen or if they develop a fever. If this occurs then the patient is asked to contact the clinic immediately at which time a formal reassessment will occur and if needed oral antibiotics can be prescribed. The patient is also warned that following any injection they may notice a short-term worsening or flare in their symptoms after the local anaesthetic has worn off (4-5 hours). This may last for 3-5 days and the patient is advised to consider icing of the area using an ice pack for 10-15 minutes every hour as required.
If non-surgical treatments fail to provide adequate relief, surgery may be considered.
Surgery is typically considered for patients with severe ankle osteoarthritis that significantly impacts their quality of life and limits their ability to perform daily activities, who have failed conservative management.
Additional tips for managing ankle osteoarthritis pain: